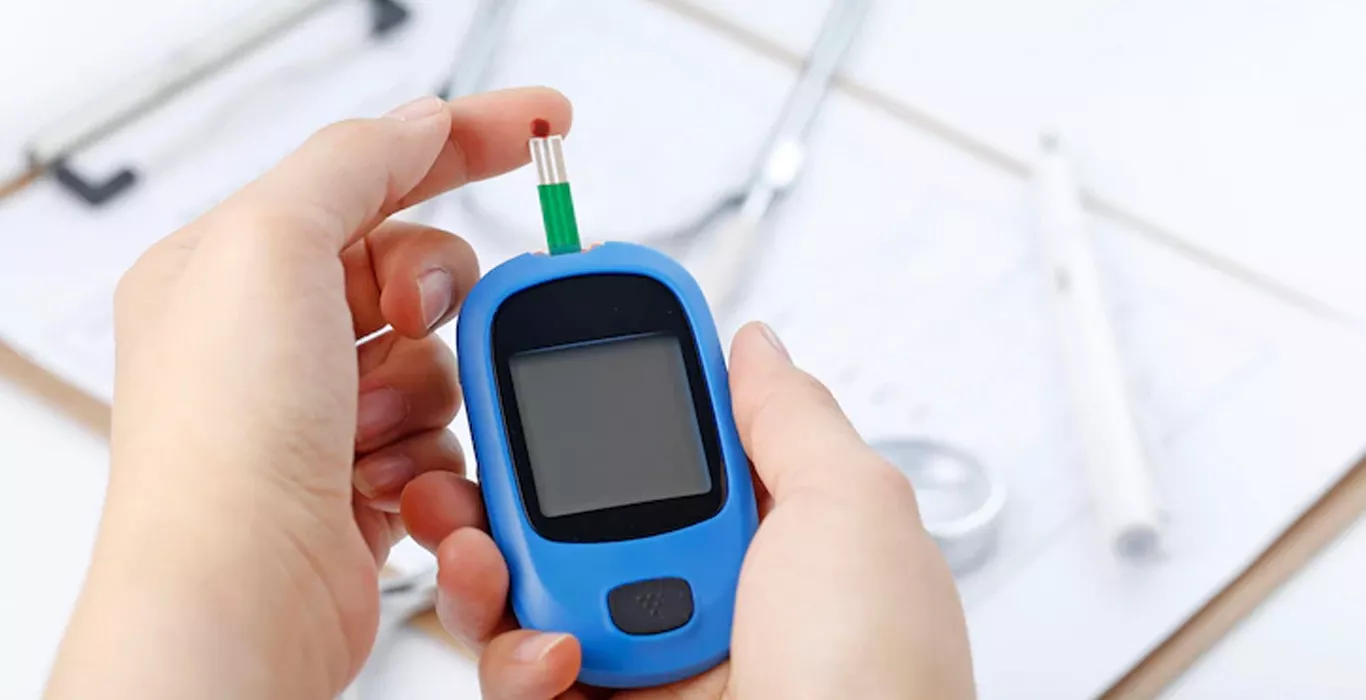
If you are a woman with type 1 diabetes and getting pregnant or perhaps wondering how to get pregnant with diabetes type 2 or simply thinking is it hard for diabetics to get pregnant. Then the following chapter which is an excerpt from the discourse conducted for the benefit of all of you by Dr. Jyoti Gupta ( Indira Infertility Clinic and test tube baby centre in Faridabad) at the Indira IVF clinic in Faridabad will certainly help you solve your queries. In this particular discourse, Dr. Jyoti Gupta ( Indira IVF Clinic in Faridabad) discusses the various studies conducted around the world about diabetes and infertility in females and also answers some questions asked by the participants relating to the above-said topic.
Diabetes and Infertility in Females
Introduction
Diabetes is an illness that has an effect on many people in addition to their family members. The WHO anticipates that over one hundred and eighty million people all around the world have got diabetic issues. This figure will probably at least increase twofold by 2030. Type 1 diabetes, which mostly has an effect on young people, is growing alarmingly around the world, at a pace of 3% each year. Some 70,000 kids aged fourteen and also under progress Type 1 diabetic issues yearly. Type 2 diabetic issues are usually growing in great number among youngsters as well as teenagers since morbid obesity levels within this populace continuously rise, in each developed as well as developing countries. All forms of diabetes have an effect on females in numerous ways, as well as one of them is going to be the highlight of the present discourse – the connection between diabetes mellitus as well as infertility explained Dr. Proshun Bera (Indira IVF centre in Kolkata).
Can diabetes cause infertility in women?
Answer: Most women with PCOS get above normal amounts of testosterone (hyperandrogenism). PCOS could affect fertility by resulting in abnormal periods (oligomenorrhea) or maybe missing periods (secondary amenorrhea). PCOS is especially connected with overweight as well as type 2 diabetic issues answered Dr. Nandini Devi ( Indira Infertility Clinic and test tube baby centre in Chennai).
Diabetes mellitus Type 1, as well as Type 2, may be used in the different medical diagnosis of menstrual irregularities as well as infertility. The reproductive time period of diabetic females might be lowered as a result of deferred menarche and then early menopause. Throughout the reproductive period, diabetic issues continue to be linked to menstrual irregularities, for instance, oligomenorrhea as well as secondary amenorrhea. This was discovered that good glycemic control together with avoidance of diabetic issues enhances all these abnormalities and also raises fertility rates near to the ones that are found in the general public. Many women with chronic menstrual irregularities in spite of sufficient therapy ought to be handled by much wider assessment, that could consist of the assessment of the hypothalamic–pituitary–ovarian axis as well as the hormonal level, existence of autoimmune thyroid illness as well as anti-ovarian autoantibodies, and even hyperandrogenism notified Dr. Jyoti Gupta ( Indira IVF Clinic in Faridabad).
Menarche and Menstrual Period Disruptions in Type 1 Diabetic issues
Before the initial inception of insulin in the medical care of Type 1 diabetic issues in 1922, menarche seldom transpired in females with having diabetes all through childhood days, so when it actually did happen, menses typically ceased. Effective conception was accomplished in merely 2% of Type 1 diabetic females. The start of insulin treatment brought about menstruation to be found in nearly all women diabetes patients, still failed to get rid of menstrual disorders. Previous scientific studies from 1954 by Bergqvist revealed deferred menarche among most women with the beginning of diabetes before menarche as well as regulated for their diabetes mellitus like outpatients, along with chronic menstrual issues staying in the 3rd as well as the 4th decade in 30% of these ladies. The occurrence associated with these issues, primarily secondary amenorrhea and also oligomenorrhea, was proven to be three-times far more regular when compared with nondiabetic controls in the research by Rzepka in 1977 mentioned Dr. Nandini Devi ( Indira IVF centre in Chennai).
Succeeding epidemiologic scientific studies reinforced the point that medical diagnosis of Type 1 diabetic issues before menarche, especially before ten years of age, created a delay in menarcheal age of around one year as compared to control. Comparable end results were received in scientific studies carried out in numerous demographic populations. Also, a relationship was discovered between the menarcheal age delay as well as the existence of menstrual disorders. discovered menstrual irregularities to be two times quite as regular in diabetic females as compared to nondiabetic settings (21.6 versus 10.8%), that is less than as per Begqvist, yet no less troublesome added further Dr. Jyoti Gupta ( Indira IVF Clinic in Faridabad).
Can you get pregnant if you have type 1 diabetes?
Answer: Yes, if you gain control over your current glucose levels before pregnancy as well as during maternity. A research completed in Australia verified that ladies with type 1 diabetes mellitus who seek advice from an infertility specialist prior to having a child have a lot more potential for an effective conception. Being one of the best IVF hospitals in Faridabad our IVF specialists in Faridabad are quite adept at handling fertility cases related to diabetic issues. Since we know that the primary factor for type 1 diabetic sufferers is the fact that when they contemplate conception, they need to ensure blood glucose control is definitely under ideal circumstances advised our IVF specialist in Faridabad Dr. Jyoti Gupta ( Indira IVF centre in Faridabad).
Hypothalamic Anovulation in addition to Type 1 Diabetes
The above-explained suggestions might reveal a basic disorder of the hypothalamic–pituitary–ovarian (HPO) axis. The impact of Type 1 diabetic issues on the reproductive endocrine axis could be conceptualized like anorexia-like hypothalamic anovulation. Diabetic females with lower BMI usually tend to need menstrual disorders. You will find catabolic procedures in very young diabetic girls as well as dietary constraint results in intracellular deprivation, particularly before the medical diagnosis and also instigate insulin treatment. This might eventually result in a loss in the hypothalamic pulsatile secretion of gonadotropin-releasing hormone (GnRH), with a subsequent decline in gonadotropins secretion informed Dr. Sagarika Aggarwal ( Indira IVF centre in Lajpat Nagar).
In diabetic animal scientific studies carried out by Johnson together with Sidman in 1979, it emerged that the primary etiologic elements connected with damaged hypothalamus–pituitary operation was, in fact, deficient discharge of GnRH and/or decrease in the level of sensitivity of the pituitary gland to GnRH. Scientific studies in females by Djursing et al. in 1983 and then 1985 found reduced basal levels of luteinizing hormone (LH) in Type 1 diabetes patients with amenorrhea, and also revealed diverse responses of LH to exogenous GnRH, hence recommending that menstrual disruptions in Type 1 diabetes patients are primarily of hypothalamic beginning as opposed to key pituitary disorder stated our infertility specialist in Faridabad Dr. Jyoti Gupta ( Indira IVF Clinic in Faridabad).
The neuroendocrine regulation also needs to be looked at while explaining disruptions in the HPO axis. That it was as outlined by Djursing that Type 1 diabetic females have reduced basal prolactin ranges, not connected to the existence of menstrual issues. Nevertheless, primarily diabetic amenorrheic individuals have a reduced prolactin reaction to dopamine antagonists. These types of outcomes recommend that diabetes patients with menstrual problems could have enhanced the principal dopaminergic process, which often prevents GnRH secretion. Endogenous opioid-like peptides – endorphins – also provide an inhibitory impact on GnRH issue. It is actually considered that gonadotropin secretion is controlled by an encounter between dopamine together with endogenous opioids. Nonetheless, an earlier research by O’Hare et al. in 1987 unable to establish an alteration of gonadotropic stages or perhaps start of menstruation after intake of the opioid inhibitor naloxone in hypogonadotropic amenorrhea Type 1 diabetic females. At last, a relationship between Type 1 diabetic issues as well as polycystic ovary syndrome (PCOS) was disclosed in a fairly recent research by Codner et al. All these experts discovered that active treatment with insulin, often used in Type 1 diabetic issues so as to stop diabetic issues, may result in supraphysiological doses of insulin, eventually starting hyperandrogenism as well as PCOS . Along with exogenous hyperinsulinism, insulin resilience is usually feasible in females with Type 1 diabetes mellitus, because of reduced glucose uptake by the muscle tissue. That additionally plays a part in the growth and development of androgen surplus in females with Type 1 diabetes mellitus. Codner et al. found higher levels of complete and even free testosterone, elevated LH to follicle-stimulating hormone ratio, much larger ovarian quantities as well as irregularities in ovarian morphology. It was particularly notable among females with the start of Type 1 diabetes mellitus before menarche. PCOS occurrence of 31 in addition to 40% was recorded utilizing the Androgen surplus society standards as well as Rotterdam standards, respectively; among Type 1 diabetic ladies in Codner’s research included Dr. Jyoti Gupta ( Indira IVF centre in Faridabad).
Association between Type 2 Diabetes mellitus and Fertility
Almost all of the Type 2 diabetes mellitus women patients are postmenopausal females, however with altering nutritional as well as lifestyle patterns, the prevalence of obesity is growing, hence increasing the occurrence of Type 2 diabetes mellitus throughout the reproductive years explained Dr. Nirmal Bhargava ( Indira IVF Clinic in Rohini).
There is certainly a relationship between Type 2 diabetes mellitus as well as fertility, modifications in the period of the menstrual cycle, along with the age of the beginning of the menopause. This relationship might be described by connecting this illness to PCOS, the most frequent hormonal condition among ladies of reproductive age group, as well as a major source of infertility. Insulin resilience, morbid obesity and also diabetes mellitus clearly associate with PCOS. Both of them PCOS, as well as Type 2 diabetes mellitus, get the identical risk issues, like high blood pressure, morbid obesity, dyslipidemia and also hyperinsulinemia.
Legro et al. revealed that PCOS ladies face a considerably enhanced threat for weak glucose persistence and also Type 2 diabetic issues at all weights and also at a young age group. They even discovered that these kinds of occurrence rates are identical in 2 populations of PCOS females with totally different weights, proposing that PCOS might be a far more crucial risk element compared to ethnicity or even race for glucose intolerance in younger ladies. By difference, a research by Amini et al. revealed that PCOS is definitely widespread in Type 2 people with diabetes added further Dr. Jyoti Gupta ( Indira IVF centre in Faridabad).
Being overweight is prevalent in each PCOS as well as Type 2 diabetic female. Research has shown that overweight females planning being pregnant encounter more time to conceiving, not connected to your age as well as to cyclic frequency that is suggestive of modifications in ovarian functionality all through the periconceptional time period. Metwally et al. discovered that oocytes from females with higher BMI gave rise to blastocysts of lower quality. A current research offered a study of the ovarian follicular condition of females across a significant array of BMIs, by calculating follicular fluid hormones as well as metabolites, and granulosa together with cumulus cellular gene expression. The research exhibited increased intrafollicular insulin as well as triglycerides and even improved expression of lipoprotein receptors in obese as well as overweight ladies. Gene expression modifications were not influenced by BMI. Additionally, there was clearly a rise in free androgen profile within the ovarian follicles of overweight females, and an improved volume of C-reactive proteins, which might be connected with the lower reproductive results usually noticed in these affected individuals.
Eventually, methodical analysis of conception and fertility following bariatric surgical treatment revealed that normalization of sex hormones in addition to menstrual abnormalities, and development in PCOS, has happened described Dr. Arvind Vaid (Indira IVF Clinic in Patel Nagar, Delhi).
Can you get pregnant if you have type 2 diabetes?
Answer: A normal conception is without a doubt feasible with diabetes mellitus; however, it requires additional health care. If you are planning to have maternity with type 2 diabetic issues, refer to our fertility specialist. As well as, needless to say, a healthy diet plan not to mention physical exercise is important to facilitate control blood sugar levels. When you have your child, you could breastfeed, if you choose to answered Dr. Jyoti Gupta ( Indira IVF centre in Faridabad)
Can a baby get diabetes from the mother?
Answer: When the diabetes mellitus is poorly managed in pregnancy, the child is subjected to excessive glucose levels. This could have an effect on the child as well as mother throughout the maternity, during the time of birth, as well as after delivery. Children who definitely are born to moms with diabetes mellitus are usually bigger than some other children replied Dr. Rekha Brar ( Indira IVF Clinic in Dr. Dwarka).
What is the best diet for a pregnant woman with diabetes?
Answer: Have an excellent morning meal. Your current blood glucose amounts are most certainly to be away from whack each morning. To maintain your current level in a more healthy range, you might have to restrict carbohydrates (bread, cereal, fruits, and also whole milk), enhance your own protein (eggs, cheese, peanut butter, nut products), and also perhaps stay away from fruits as well as fruit juice completely advised Dr. Jyoti Gupta ( Indira IVF centre in Faridabad).
Relationship of Advanced Treatment of Diabetic issues Mellitus Type 1 with Decline in Infertility
In earlier times, the partnership between menstrual disorders as well as diabetic control was regarded as debatable. Kajer et al. revealed a relationship between lower BMI, higher levels of HbA1C as well as the existence of menstrual abnormalities. Yeshaya et al. discovered that patients with diabetic problems needed a greater occurrence of menstrual irregularities as compared to people with diabetes without issues. Schroeder et al. analyzed the association between the level of glycemic control in Type 1 diabetic teenagers as well as menstrual control. They revealed that more restrictive glycemic regulation, assessed by reduced amounts of HbA1C, was connected with enhanced menstrual control. Further scientific studies did not succeed to establish an important relationship with the metabolic condition (higher BMI, microvascular as well as macrovascular issues, or even higher HbA1C. Right now there have even recently been records proposing sound metabolic control among ladies with oligo/amenorrhea included our infertility specialist in Patna Dr. Anuja Singh (Indira IVF centre in Patna).
The initial population-based epidemiological research on fertility levels with time among females with Type 1 diabetes mellitus was carried out in Sweden throughout 1965 to 2004. The research followed up on 5978 Type 1 diabetic females identified at sixteen years of age group or even younger, who were discovered in the Swedish Inpatient Record, until 48 years of age, death or simply emigration. A standardized fertility ratio (SFR; the ratio of identified to anticipated amount of live births, with 95% CIs), was accustomed to convey the pertinent fertility rate. A number of live births were 4013, that was less than anticipated (SFR 0.80 (95% CI: 0.77–0.82)). The very low SFRs were noticed among ladies who got their very first hospitalization for diabetes mellitus in the primary years. SFRs improved monotonically with the calendar year of very first hospitalization to become statistically indistinguishable from 1.0 after 1984. The existence of diabetic micro vascular or simply cardio problems was connected with specifically lower fertility, primarily irrespective of year of initial hospitalization informed our IVF specialist in Pune Dr. Amol Lunkad ( Indira IVF Clinic in Pune).
In general, fertility among Type 1 diabetic females was lowered by 20% in this particular research, when compared with the paired to common Swedish women populace, with the lower SFRs in the past years. It was accompanied by a substantial rise in SFR until normalization among females with less complicated illness as well as an onset in the past twenty years. The rise in fertility after 1985 was independent of difficulty level, age at the outset hospitalization or even duration of diabetes mellitus, therefore, was most likely related to much better interventions in treatment method. Even though development was apparent irrespective of the status of diabetes mellitus issues, females with problems usually experienced reduced fertility as compared to those without these kinds of issues. The end results of this research recommend that the stricter metabolic control worked out for the past twenty years, along with much better control over blood pressure levels and regular usage of medicines active in inhibiting the renin–angiotensin process, in addition, has also been effective pertaining to conserving fertility Dr. Ishita Lunkad ( Indira IVF centre in Pune).
The menopause
It is recognized that affected individuals with diabetes mellitus encounter alterations of cellular senescence sooner than the common population. This might show that one these symbol of maturing in females, the menopause, might happen before as compared to nondiabetic ladies described Dr. Jyoti Gupta ( Indira IVF Clinic in Faridabad).
A research carried out by Dorman et al. among Caucasian ladies with Type 1 diabetes mellitus when compared the age at the menopause of 143 ladies with Type 1 diabetes mellitus, to their non-diabetic sisters and also completely unrelated noniabetic controls. They discovered that the average age was considered young for Type 1 diabetic females. Ladies with Type 1 diabetes mellitus were around two times just as prone to have observed the menopause sooner than comparable non diabetic females. Particularly, affected individuals with earlier menopause were young at Type 1 diabetic commencement (8.6 versus 12.6 years of age; p = 0.10). Multivariate evaluation established that Type 1 diabetic issues were a completely independent determining factor of earlier menopause (HR: 1.98; p = 0.056). At the same research, the age group of menarche was identified to be considerably more mature for Type 1 diabetic females as compared to non-diabetic ladies; taken along with early menopause, this consequently lowers the reproductive time period in Type 1 diabetic females by six years added Dr. Priyanka Kasriwal ( Indira Infertility Clinic and test tube baby centre in nashik).
Strohmeyer et al. discovered the age group of organic menopause in Type 1 diabetic females to be practically ten years prior as compared to non-diabetic sisters as well as not connected non-diabetic controls. The average age group of self-reported all natural menopause in Type 1 diabetic females was 42 years, yet perimenopausal signs or symptoms were now noticed in ladies in their thirties as well as forties. Early menopause in Type 1 diabetic females can also be associated with the autoimmunity issues with Type 1 diabetes mellitus. Goswami et al. discovered greater occurrence of thyroid peroxidase autoantibodies in affected individuals with premature ovarian failure as compared to healthy and balanced controls. The potential autoimmune etiology of infertility linked to Type 1 diabetes mellitus is going to be outlined in the next paragraphs explained Dr. Mayuri Assudani( Indira IVF centre in Nagpur).
Autoimmunity
Autoimmune ailments, such as oophoritis, orchitis as well as underactive thyroid, are well-established reasons for infertility. Autoimmune oophoritis may well happen as an element of type I as well as type II syndromes of polyglandular autoimmune malfunction, that are connected with autoantibodies to many endocrines as well as other bodily organs. Younger ladies with normal premature ovarian failure face an improved threat of autoimmune hypothyroidism as well as ought to be examined for this disease.
Type 1 diabetes mellitus and also autoimmune thyroid ailments often manifest jointly within family members as well as in the very same individual. Hence, we could believe that sufferers with Type 1 diabetes mellitus which have overt or even disguised underactive thyroid can also be in danger of premature ovarian failure. Generally, assessment of premature ovarian failure must consist of serum level of follicle-stimulating hormone and also estradiol and even verification for asymptomatic autoimmune adrenal inadequacy, because it is much more frequent in females with autoimmune ovarian failure. Also, the assessment must consist of thyroid-stimulating hormone, free T4, antithyroid-peroxidase, antithyroglobulin antibodies as well as karyotype educated Dr. Kanika Kalyani ( Indira IVF Clinic in Mumbai).
Menstrual period alterations noticed in affected individuals with Hashimoto’s thyroiditis consist of menorrhagia, even more, recurrent as well as extended periods, as well as dysmenorrhea. The occurrence of thyroid autoimmunity is substantially greater among infertile females compared to among fertile females, particularly amongst those whose infertility is due to endometriosis or even ovarian irregularities. In an investigation carried out by Strotmeyer et al. over 40% of females with Type 1 diabetes mellitus experienced Hashimoto’s thyroiditis. However, he could not find menstrual issues to be considerably influenced by Hashimoto’s thyroiditis. It might be believed that in a few of the females, Hashimoto’s thyroiditis was analyzed a lot later on after menstrual issues transpired. Some others needed their thyroid ailment under appropriate control and then were not as likely to display menstrual disorders.
Snajderova et al. investigated the existence of organ-specific autoantibodies as well as other endocrine autoimmune issues in women with Type 1 diabetes mellitus They discovered ovarian autoantibodies in 67.9% of Type 1 diabetic women compared to 4.8% of nutritious regulates (p < 0 .01). Autoantibodies guided to ovarian steroid-producing body cells were recurrent in diabetic women with both equally abnormal as well as regular menstrual periods. The function of thyroid participation in diabetes mellitus Type 1 affected individuals, as well as their effects on menstruation period as well as fertility, continues to be clearly identified spelled out Dr. Amol Naik ( Indira IVF centre in Navi Mumbai ).
Sexual Irregularities and Diabetes mellitus
It is actually long been anticipated that around 35–75% of adult males with diabetic issues will certainly experience some level of erectile disorders through their lifespan. They are inclined to cultivate erectile disorders 10–15 years sooner than adult males without diabetes mellitus. The consequence of diabetes mellitus on women sexual performance was not entirely identified and also resolved in past times. Enzlin et al. examined fifteen scientific studies carried out between 1971 as well as 1996, and even recorded that the occurrence of damaged sexual arousal and also insufficient lubrication was between 14–45% among diabetic females, substantially greater than in healthy controls. In a succeeding regulated research which they carried out in 2002, Enzlin et al. discovered that much more females with diabetes mellitus compared to control subjects disclosed sexual disorders (27 versus 15%; p = 0 .04). Women sexual disorders might have a subordinate impact on fertility by lowering sexual desire as well as restraining sexual activity, particularly around the period of ovulation informed Dr. Santosh S Daaphle ( Indira IVF Clinic in Kolhapur).
Conclusion
Enhanced glycemic control was discovered to be connected with progress in menstrual irregularities as well as in fertility levels. Nonetheless, a few people with diabetes encounter continual menstrual disorders although good quality metabolic regulation is accomplished. In those affected individuals, it really is advisable to deal with the potential irregularities in the HPO axis in order to examine their hormonal level (GnRH, LH, follicle-stimulating hormone and also GnRH stimulus check), along with the autoimmune etiology linked to diabetes mellitus concluded Dr. Jyoti Gupta ( Indira IVF centre in Faridabad).
Comments
Articles
2023


Female Infertility Male Infertility
How many days Sperm Live in Female Body after Intercourse?
While it depends on the correct circumstances and the stage of the woman's men...
2023


What Causes High Estrogen in Women
Estrogen is a very important hormone in a female’s body. It is especially ne...
2022


Female Infertility Infertility Tips
Why do You Need Fertility Treatment
As we all know infertility rate is constantly rising in our society day by day...
2022


Female Infertility Infertility Tips
The Impact of Covid-19 on Pregnant Women & their Babies
Pregnant women and those in close-contact with them must take necessary precau...
2022

Female Infertility Infertility Tips
Is Covid-19 Vaccination dangerous for pregnant women? Know the Benefits and Risks
What do we know today about the benefits and risks of vaccination in pregnant ...
2022


Female Infertility Infertility Tips
What every young woman of today needs to know
A lot of people get themselves examined once or twice a year by their doctor. ...
2022


Female Infertility Infertility Tips
Do Infertile Women Menstruate?
It is a common belief over decades that women with normal menstrual cycle patt...
2022


Female Infertility Infertility Tips
We have sexually satisfied life , Still can we be infertile ?
Infertility is inability to conceive after one year or more with regular unprote...
2022


Infertility Tips Female Infertility
Should women go for IVF treatment?
Incidence of infertility in India is 10 to 15%, in other words 27.5 million co...
2022


Infertility Tips Female Infertility
IVF protocols for women with low ovarian reserve
Epilogue – low ovarian reserve Whenever we come across women with low ova...
Tools to help you plan better
Get quick understanding of your fertility cycle and accordingly make a schedule to track it